————
Information and Pictures on Pelvic Inflammatory Disease (PID), a condition usually caused from sexually transmitted diseases. Information including symptoms, diagnosis, treatment, transmission, prevention and other general information.
—————-
Pelvic Inflammatory Disease (PID) is a progressive infection and inflammation, which can result in substantial damage to a woman’s reproductive system. Many different organisms can cause Pelvic Inflammatory Disease, but most cases are usually caused by the bacteria:
Both may occur together.
It has been shown that:
- bacteria normally present in small numbers in the vagina and cervix may play a role.
- various other germs are sometimes involved.
- 20% of patients with Pelvic Inflammatory Disease (PID) have no definite cause.
Pelvic Inflammatory Disease (PID) usually occurs in sexually active women between the ages of 15-25 and the highest rate of infection is among teenagers and adolescents. More than 750,000 new cases of Pelvic Inflammatory Disease (PID) are diagnosed every year in the U.S.
The cervix usually prevents bacteria in the vagina from spreading up into the internal organs but if the cervix is exposed to a sexually transmitted disease (STD), such as Gonorrhea or Chlamydia, the cervix becomes infected.
The gonococcus bacteria, Neisseria gonorrhea:
- moves upwards to the fallopian tubes, where it casts out some cells and invades other cells
- multiplies within and beneath these cells
- spreads to other organs resulting in more inflammation and scarring
Chlamydia trachomatis and other bacteria may behave similarly.
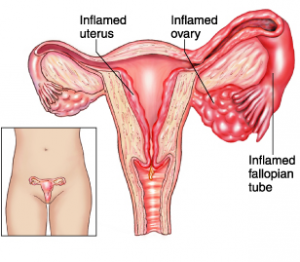
The internal organs can become inflamed and infected if the disease travels, often damaging the fallopian tubes making it difficult to become pregnant.
———–
Pelvic Inflammatory Disease Symptoms
Pelvic Inflammatory Disease (PID) occurs in:
- the fallopian tubes
- the lining of the uterus
- the ovaries
- the upper genital tract
- the uterus
- throughout the pelvic area
Whether treated or untreated, Pelvic Inflammatory Disease (PID) can result in:
- chronic pain
- ectopic pregnancy (pregnancy outside the womb)
- fever
- scarring
- sterility
- swelling
Symptoms
- abnormal or unusual vaginal discharge (yellow or green color with an unusual odor)
- abnormal vaginal bleeding
- dull pain and tenderness in the stomach
- lower abdominal or pelvic pain
- pain during urination
- painful intercourse
- pain in the anus/rectum
- pain in the lower abdomen and back
- raised temperature and fever
- right upper abdominal pain
- similar signs and symptoms to that caused by a number of different bacteria
Various menstruation problems can occur:
- irregular periods
- spotting or cramps throughout the month
- unusually long or painful periods
The following symptoms occur if the infection has spread to the lining of the abdomen:
- chills
- high fever
- nausea
- vomiting
Pelvic Inflammatory Disease (PID) when caused by the Chlamydia bacteria may result in only minor symptoms, sometimes with no symptoms at all, even though it can seriously damage the reproductive organs
Symptoms of Pelvic Inflammatory Disease (PID) caused by the Gonorrhea bacteria often begin immediately after menstruation rather than at any other time during the menstrual cycle. This has not been proved in Chlamydial Pelvic Inflammatory Disease (PID)
Note
- As the symptoms of Pelvic Inflammatory Disease (PID) can sometimes be confused with those of appendicitis and other infections, it is VERY IMPORTANT to see a doctor immediately if you have any of the above symptoms
- Waiting even 1-2 days can allow the infection to spread farther into your body and cause more pain and damage
————-
Photos of PID Symptoms———
Pelvic Inflammatory Disease Transmission
The sexually transmitted infections that most commonly cause Pelvic Inflammatory Disease (PID) are:
These diseases are carried in the semen and other body fluids of infected people and are spread to the woman’s cervix during sexual contact.
The disease infects:
- abdomen
- anus
- fallopian tubes
- glands at the opening of the vagina
- ovaries
- urethra (passageway for urine)
- uterus
Pelvic Inflammatory Disease (PID) is not always the result of an STD Infection.
Other causes include:
- a germ (microbe) which is transmitted sexually
- childbirth
- normal bacteria in the vagina sometimes spreads into the uterus, fallopian tubes and abdomen, causing Pelvic Inflammatory Disease (PID)
- spread of a germ from a nearby organ, as in appendicitis
- spread of an infection in the blood stream from other parts of the body
Certain surgical procedures on the female organs may cause this condition, such as:
- abnormal Pap smear
- after the insertion of an intrauterine device (IUD)
- dilatation and curettage (D & C)
- therapeutic abortion/medical termination of pregnancy
Risk Factors
- a prior episode of Pelvic Inflammatory Disease (PID), because the body’s immune system is often damaged during the initial bout of upper genital tract infection
- multiple sex partners
- sexually active teenagers are more likely to develop Pelvic Inflammatory Disease (PID) than older women
- use of a contraceptive IUD (intrauterine device)
- women with STDs, in particular gonorrhea and chlamydia, are at greater risk of developing Pelvic Inflammatory Disease (PID)
Women who douche:
- once or twice a month may be more likely to get Pelvic Inflammatory Disease (PID) than those who douche less than once a month
- may push bacteria into the upper genital tract
- may ease discharge caused by an infection and therefore delay getting treatment
———
Pelvic Inflammatory Disease Diagnosis
The doctor or health practitioner will use one or more of the following procedures to confirm diagnosis:
- blood tests
- Culdocentesis
- culture of vaginal and cervical secretions
- laparoscopy (endometrial biopsy)
- microscopic examination
- pelvic examination
- ultrasound scan
Culdocentesis
Fluid is removed from behind the vagina with a needle and examined for signs of bleeding or infection.
Laparoscopy (endometrial biopsy)
A small cut is made in the navel through which an optical instrument with a light is inserted to look inside the uterus to check for any abnormalities in the reproductive organs. It is possible to distinguish between Pelvic Inflammatory Disease (PID) and other serious problems that may have similar symptoms to Pelvic Inflammatory Disease (PID). Samples for cultures or microscopic studies are also obtained.
Microscopic examination
A mucus sample is taken from inside the vagina and inside the neck of the womb with a swab and sent to the laboratory to look for microbes. These will be examined under a microscope for gonorrhea and chlamydial infection.
Pelvic examination
If a physical examination is carried out, the doctor will require a detailed history of the woman’s health and sexual activity and should also check for:
- abnormal vaginal or cervical discharge
- cervical chlamydial infection or gonorrhea
- fever
- lower abdominal pain
- pain or abdominal tenderness when the cervix is touched or moved
Diagnosis of gonorrhea or Chlamydia with pelvic pain or cervical motion tenderness sometimes confirms the diagnosis.
Ultrasound Scan
Sound waves are used to form an image of the reproductive organs and the womb, ovaries and other organs in the pelvis, which enables the doctor to distinguish between Pelvic Inflammatory Disease (PID) and other serious problems with similar symptoms.
Screening
Screening and and treatment of women who unknowingly had chlamydial infection reduced cases by more than 60%.
—–
Pelvic Inflammatory Disease Research
New diagnostic tests are being developed, particularly to diagnose the infection in women with asymptomatic (silent) Pelvic Inflammatory Disease (PID).
Topical microbiocides and vaccines to prevent gonorrhea and chlamydial infection are being developed.
A suppository containing lactobacilli, the normal bacteria found in the vaginas of healthy women, is being tested as these bacteria colonize the vagina and may be associated with reduced risk of gonorrhea and Bacterial Vaginosis, both of which cause Pelvic Inflammatory Disease (PID).
——
Pelvic Inflammatory Disease Treatment
- antibiotics (two or more antibiotics may be used together to affect any possible bacteria that may have caused the condition)
- bed rest
- pain killers may be advised
- sexual abstinence
- sometimes intravenous (IV) treatment is required
Even if the symptoms cease you should finish the full treatment regimen.
Surgery may be needed to:
- remove abscesses
- remove scar tissue
- repair or remove reproductive organs
Hospitalization may be recommended if the patient:
- cannot take oral medication
- does not respond to treatment after a few days
- has an abdominal emergency, such as appendicitis
- has an uncertain diagnosis
- has a severe initial presentation
- is an adolescent under the age of 18
- is infected with HIV
- is pregnant
- is severely ill
- needs intravenous antibiotics
—–
Pelvic Inflammatory Disease Prevention
Help Factors
- abstinence from sexual intercourse
- avoiding multiple sexual partners
- avoiding sexual contact with people at risk of infection
- getting early treatment which may prevent the development of Pelvic Inflammatory Disease (PID)
- using latex condoms and other barrier contraception can usually protect against infections associated with Pelvic Inflammatory Disease(PID) and prevent transmission of the bacteria from one person to the next
Risk Factors
- birth control pills, injections and implants do not protect against the transmission of Pelvic Inflammatory Disease (PID) and other sexually transmitted diseases (STDs)
- sexual contact with multiple partners
- unsafe sexual practices
It is very important for women to:
- discuss with partner any risk factors
- notice any signs of discharge with odor or bleeding between cycles, which could indicate infection
Because men are often silent carriers of these bacteria, the male partner of a woman diagnosed with Pelvic Inflammatory Disease (PID) should see a doctor or health professional to be examined and checked for a sexually transmitted disease.
In the event of Chlamydia or Gonorrhoea or any other sexually transmitted diseases being diagnosed it is important to contact any persons with whom you have been sexually involved so they may be diagnosed and given treatment if required. This is essential to prevent further unnecessary spread of the bacteria.
Tracing sexual contacts is carried out:
- very professionally
- with discretion
- with sensitivity
————
Pelvic Inflammatory Disease Prognosis
After having Pelvic Inflammatory Disease (PID):
- 9% of women have ectopic pregnancies.
- 10-30% of women will lose the ability to become pregnant after just one episode of Pelvic Inflammatory Disease (PID).
- 15% of all infertile women are infertile because of tubal damage caused by Pelvic Inflammatory Disease (PID).
- 18% of women develop chronic pelvic pain.
- scarring will cause approximately 20% of women to become infertile.
Ectopic Pregnancy
After having Pelvic Inflammatory Disease (PID) a small percentage of women develop scarred fallopian tubes, which can cause difficulties with falling pregnant in the future.
The risk of an ectopic pregnancy increases due to the changes in the normal anatomy of the woman’s genital tract caused by Pelvic Inflammatory Disease (PID). An ectopic pregnancy is where an embryo grows outside of the uterus.
If not rapidly diagnosed an ectopic pregnancy can cause:
- abscesses
- infertility (an inability to get pregnant)
- internal bleeding
- long-term pelvic pain
- repeat bouts of illness
- rupture of the fallopian tube
- severe pain
- shock and death of the mother (it is the leading cause of pregnancy-related death in African-American women)
Other Complications
Women with recurrent episodes of Pelvic Inflammatory Disease (PID) are more likely than women with a single episode to suffer scarring of the tubes that leads to:
- chronic pelvic pain
- infertility
- problems in infants born to affected women
- tubal pregnancy
With each episode of re-infection the risk of infertility is increased.